New Guidelines Are ‘Huge News’ in Stroke Care
April 15, 2026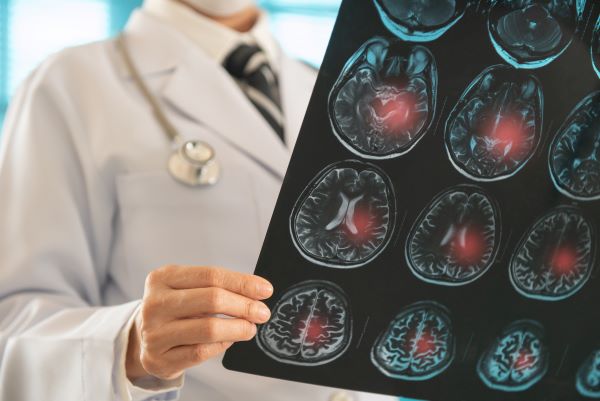
If you think you or someone else may be having a stroke, don’t wait—call 911 immediately.
Stroke treatments that have saved countless lives and prevented untold disabilities are now available to more patients than ever. And Kasim Qureshi, MD, a neurologist and vascular neurologist with Trinity Health Medical Group, Neurology, could not be happier about the change.
It’s huge news. It’s immensely positive,” he said.
“Stroke Awareness Month in May reminds us that this is one of the leading causes of death and disability. People’s lives are changed forever after having a stroke. So these changes really can't be overstated.”
The changes arrived earlier this year: the first updates since 2019 to American Heart Association guidelines for ischemic strokes, which are caused by blood clots and account for 87% of all strokes.
Dr. Qureshi cited three key points from the guidelines:
- Clot-dissolving medicine TNK can now be given to select patients up to 24 hours from the first symptoms, instead of being limited to the first 4.5 hours.
- Taking an individualized approach makes more patients, even some with recent surgeries or on blood-thinners, eligible to receive TNK.
- More patients are now eligible to receive thrombectomies, minimally invasive procedures that physically remove clots from the brain.
One thing that has not changed? Patients still must recognize the signs of stroke and seek help immediately. But when they do, neurologists like Dr. Qureshi now have more options to help them.
Old precautions, new potential for medications
Doctors have been treating stroke patients with clot-dissolving medications — the most common type now used in the United States is TNK (Tenecteplase) — since 1995. But guidelines initially restricted the window for use to three hours from the first symptoms. That was because these powerful medications prevent the body from forming blood clots.
“And particularly when you’re having a stroke, that part of the brain starts dying out and disintegrates, so it's susceptible to bleeding as it is,” Dr. Qureshi said. “So the longer you go with the stroke and the later you give a medication like TNK, the more you increase the risk of bleeding.”
Later studies expanded the window to 4.5 hours. Then clinical trials in past five years indicated the medications could be used up to 24 hours after symptoms in some patients.
Similarly, research has shown that TNK may be suitable even in cases where it previously was withheld out of an abundance of caution. Examples include someone who recently had surgery, or somebody using blood thinners. The new guidelines call for individualized risk assessments.
“We were restricted in the use of this medication because we didn't have good evidence to do so,” Dr. Qureshi said. “So now that we finally have the evidence, it's a huge change.”
One that could have a profound impact on the lives of some patients, he said.
“When you look at stroke patients who have received TNK versus those who have not, three months out from their stroke, the patients who receive the medication have a lower degree of disability,” he said. “And that could be something like ability to walk or ability to speak or ability to eat without needing a feeding tube.”
More applications for ‘truly remarkable’ procedure
Another advancement in stroke treatment arrived in 2015. With thrombectomies, an interventional neurologist or neurosurgeon uses a wire entered in the groin or wrist to follow arteries to the brain, allowing physical removal of the clot. This procedure may be necessary for large clots or those that can’t be resolved by medication alone.
“And it’s one of the most remarkable procedures in all of medicine. I’m a little bit biased as a stroke doctor, but it’s truly remarkable,” Dr. Qureshi said. “These patients come in with huge, massive strokes, completely paralyzed, unable to speak, unable to see, and we take them for a thrombectomy. And after the thrombectomy, they are normal. That's how remarkable these procedures are.”
The good news is that the new guidelines recognize that more stroke patients than previously thought could benefit from thrombectomies, he said.
And as someone who has been involved in stroke clinical trials since he was in high school, Dr. Qureshi expects progress on stroke care to continue.
“You’re probably looking at about a hundred really high-quality studies that are published every year looking at stroke,” he said. “So there's always incremental changes year to year. And as the evidence comes out, we do implement that in our clinical practice.”
Guideline changes are only part of the equation
Many of the changes in the guidelines came as no surprise to stroke neurologists, Dr. Qureshi said, because they follow the research closely. But he applauded the work of the panel of experts to develop unbiased new recommendations to be applied nationwide.
Putting those changes into action will require education and collaboration, he said. Stroke care involves so many different components of the health system: first responders, emergency departments, radiology, neurology and more.
“It's a very coordinated system in taking care of every single patient,” he said. “Big changes like this in stroke care always requires a lot of reorganization of our healthcare system. It requires a lot of education and a lot of behind the scenes work and how we organize our workflows in the hospital and how we arrange our systems of care.”
One of the most important elements of effective stroke treatment is how patients respond to initial symptoms. The best treatments in the world won’t help when care is delayed.
“One of the most challenging things we face as stroke neurologists is when we get a patient who has had stroke symptoms for over a day, a couple days,” Dr. Qureshi said. “Your arm is weak, your vision may be going out, and you've waited a day or so to see if it gets better and then have come in and we've found the stroke. And at that point, it’s much too late, unfortunately.”
The brain is sensitive to losing blood flow, and “every minute that your brain does not have blood flow, a million brain cells die,” he said. “The faster you get to the emergency room, the more we can do to try to stop that stroke and save your brain from having long-term damage.”
Even better is avoiding a stroke in the first place.
“Many strokes are caused by underlying medical problems, like diabetes, high blood pressure, high cholesterol, smoking. So making sure if you have any of those conditions that they’re well controlled, these are huge things that reduce your stroke and heart attack risk,” Dr. Qureshi said.
“Taking care of your underlying medical problems is huge.”
Check Your Stroke Risk
Start with a Stroke Health Risk Assessment to better understand your personal risk factors and decide next steps for your health.
If you’re concerned about your stroke risk, we recommend reaching out to your primary care provider (PCP).
Don’t have a PCP? We offer convenient primary care locations across Michigan. Whether you’re an existing patient or new to our system, you can browse providers and schedule your next appointment here.
Make an Appointment